An electrocardiogram (ECG or EKG) is one of the most commonly performed tests in medical clinics — a fast, painless, non-invasive recording of the heart’s electrical activity that provides invaluable diagnostic information about heart rhythm, rate, and structural function. Despite its simplicity, a properly interpreted ECG contains a remarkable amount of clinical information that guides cardiac diagnosis and management. This guide explains what an ECG is, how it is performed, and what it can and cannot detect.
How an ECG Is Performed
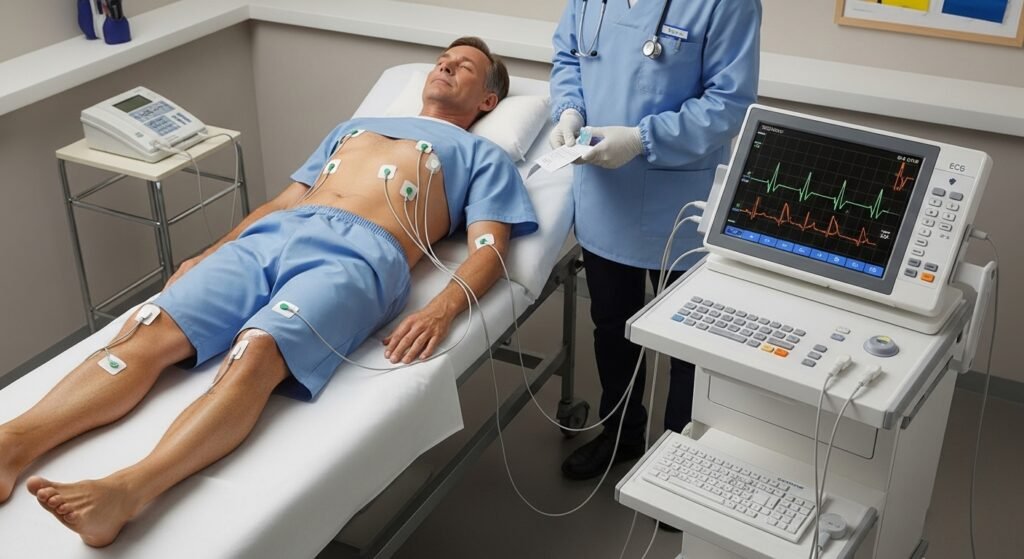
You lie flat while a technician or nurse attaches 10 electrode stickers to specific locations on your chest, arms, and legs. The electrodes detect electrical impulses generated by the heart as it contracts and relays them to the ECG machine, which records the signals as waveforms on graph paper or a digital display. The entire process takes approximately 5–10 minutes and causes no discomfort beyond the electrode adhesive.
What an ECG Reveals
Heart Rate and Rhythm
The ECG accurately measures heart rate and identifies rhythm abnormalities (arrhythmias) — including atrial fibrillation, ventricular tachycardia, bradycardia, heart blocks, and premature beats. Rhythm diagnosis directly guides treatment decisions for many cardiac conditions.
Signs of Heart Attack
The ECG is the primary rapid diagnostic tool for acute myocardial infarction (heart attack). Characteristic ST-elevation or new Q-waves indicate acute or past heart attack. Emergency ECG interpretation allows immediate reperfusion treatment (stenting or thrombolytics) within minutes of hospital arrival.
Chamber Enlargement and Conduction Defects
Left ventricular hypertrophy (from hypertension or aortic stenosis), bundle branch blocks, prolonged QT interval (a risk factor for life-threatening arrhythmia), and electrolyte disturbances producing cardiac effects are all identifiable on ECG.
What an ECG Cannot Detect
A normal ECG does not rule out heart disease. Many people with significant coronary artery disease have normal resting ECGs. The ECG captures only the moment it is recorded — intermittent arrhythmias may not be present at the time of the test. Additional testing (stress test, Holter monitor, echocardiogram) is required when clinical concern persists despite a normal ECG.
Conclusion
The ECG is an invaluable, fast, safe, and inexpensive cardiac diagnostic tool that every medical clinic should perform when clinically indicated. It takes 5 minutes and provides immediate cardiac information — its value in diagnosing heart attack, arrhythmia, and conduction disease makes it one of the most important tests in medicine.
FAQs – ECG/EKG
Q1. Is an ECG the same as an echocardiogram?
A: No. An ECG measures the heart’s electrical activity. An echocardiogram uses ultrasound to visualize the heart’s structure and function — chamber sizes, wall motion, valve function. Both provide different and complementary cardiac information.
Q2. Does a normal ECG mean my heart is healthy?
A: A normal ECG is reassuring but does not guarantee the absence of heart disease. Significant coronary artery disease, mild valve disease, and certain cardiomyopathies may produce normal resting ECGs. Clinical evaluation in context is essential.
Q3. Can I exercise before an ECG?
A: For a resting ECG, you should be at rest before the test. For a stress test (exercise ECG), you exercise during the test. Vigorous exercise shortly before a resting ECG can cause sinus tachycardia that may obscure other findings.
Q4. Why does an ECG use multiple leads?
A: The 12 standard leads view the heart’s electrical activity from 12 different angles, providing a three-dimensional picture of electrical propagation through the heart. Different leads are sensitive to different heart regions — combining them allows localization of problems to specific areas.
Q5. How often should someone get an ECG?
A: There is no recommendation for routine ECG screening in asymptomatic low-risk people. ECGs are ordered based on clinical indication — cardiac symptoms, known heart disease, evaluation before surgery, monitoring of medications affecting cardiac conduction, or hypertension-related cardiac assessment.


