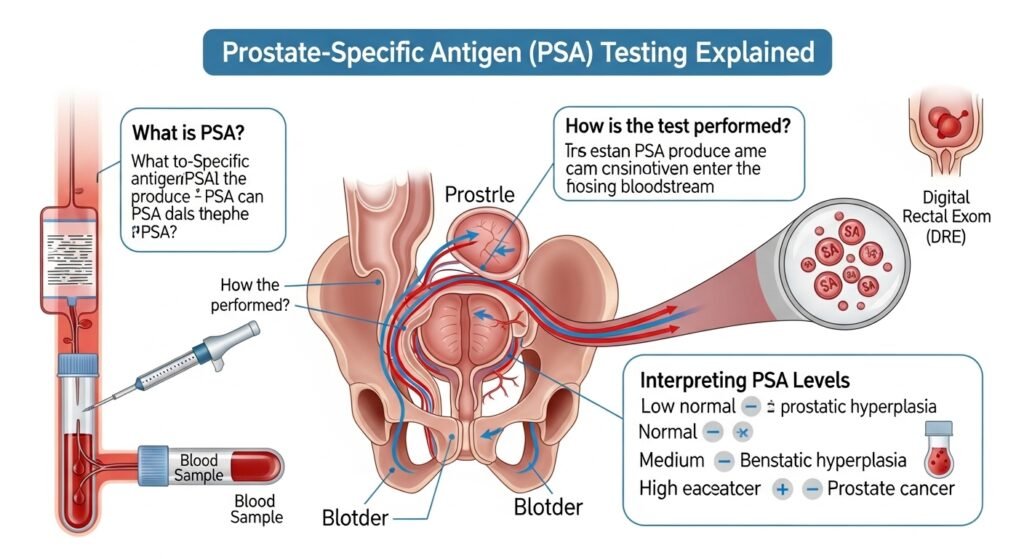
The prostate-specific antigen (PSA) blood test measures the level of PSA — a protein produced by both normal and cancerous prostate tissue — in the bloodstream. Elevated PSA can indicate prostate cancer, but also benign conditions including benign prostatic hyperplasia (BPH) and prostatitis. PSA testing has been the subject of significant medical debate — it undeniably detects more prostate cancers, but many detected cancers would never have caused harm, leading to overdiagnosis and overtreatment. Modern PSA testing involves shared decision-making that weighs these competing considerations. This guide explains PSA testing and its role in prostate cancer screening.
What PSA Levels Mean
PSA below 4.0 ng/mL has traditionally been considered normal, though this cutoff is increasingly nuanced — a rising PSA within the “normal” range may indicate developing cancer, while a PSA above 4.0 is often caused by BPH rather than cancer. PSA velocity (rate of change over time) and PSA density (PSA relative to prostate volume) provide additional diagnostic information. Age-specific PSA reference ranges account for naturally increasing PSA with aging.
Limitations and Controversies
PSA sensitivity and specificity are imperfect — many PSA elevations are from benign causes, leading to unnecessary biopsies, while some prostate cancers produce little PSA and are missed. Prostate cancer detected through PSA screening is often indolent (slow-growing and unlikely to cause harm), raising concerns about overdiagnosis and overtreatment with radiation, surgery, and their associated side effects (urinary incontinence, erectile dysfunction).
Current Recommendations
USPSTF recommends a shared decision-making conversation about PSA screening for men ages 55–69, weighing potential benefits (mortality reduction) against harms (overdiagnosis, overtreatment). Men at higher risk (African American men, those with first-degree relatives diagnosed with prostate cancer before age 65) should begin this conversation earlier, at age 40–45. Above age 70, PSA screening is generally not recommended.
Conclusion
PSA screening is a nuanced clinical decision requiring a conversation between you and your doctor about your personal values, risk factors, and preferences. Neither universal screening nor universal avoidance of screening is appropriate — shared decision-making produces the most personally relevant outcome for each individual patient.
FAQs – PSA Testing
Q1. What level of PSA is dangerous?
A: There is no single “dangerous” PSA level — even PSA above 10 ng/mL most commonly reflects benign causes. PSA is always interpreted in context: trend, rate of change, patient age, prostate size, and other clinical factors determine whether biopsy is warranted.
Q2. Can PSA be elevated for non-cancer reasons?
A: Yes. PSA is elevated by BPH (by far the most common cause of elevated PSA), prostatitis (infection or inflammation), recent ejaculation (within 24–48 hours), prostate manipulation (digital rectal exam, cystoscopy), bicycle riding, and vigorous perineal exercise.
Q3. What happens after an elevated PSA?
A: Depending on degree of elevation and clinical context, options include repeat PSA (ruling out transient elevation), additional biomarker testing (Prostate Health Index, 4Kscore, PSAD), MRI of the prostate (identifying suspicious areas for targeted biopsy), or prostate biopsy. Your urologist or primary care doctor guides this pathway.
Q4. Does finasteride affect PSA levels?
A: Yes. 5-alpha reductase inhibitors (finasteride, dutasteride) used for BPH or hair loss reduce PSA levels by approximately 50%. When monitoring PSA in patients on these medications, PSA values should be doubled for interpretation purposes. Failure of PSA to decline as expected on these medications warrants investigation.
Q5. How is prostate cancer treated?
A: Treatment depends on cancer grade, stage, patient age and health. Low-risk cancers may be managed with active surveillance (monitoring without immediate treatment). Intermediate and high-risk cancers are treated with radical prostatectomy, radiation therapy (external beam or brachytherapy), and/or hormone therapy. Treatment selection involves urologists, radiation oncologists, and patient preferences.