Peripheral neuropathy — damage to peripheral nerves causing numbness, tingling, pain, or weakness in the extremities — is one of the most common neurological conditions, affecting approximately 20 million Americans. Nerve conduction studies (NCS) and electromyography (EMG) are the primary diagnostic tests used at neurology and neuromuscular clinics to objectively assess peripheral nerve and muscle function, identifying the specific pattern of nerve damage and guiding diagnosis and management. This guide explains nerve conduction testing and its clinical applications.
How Nerve Conduction Studies Work
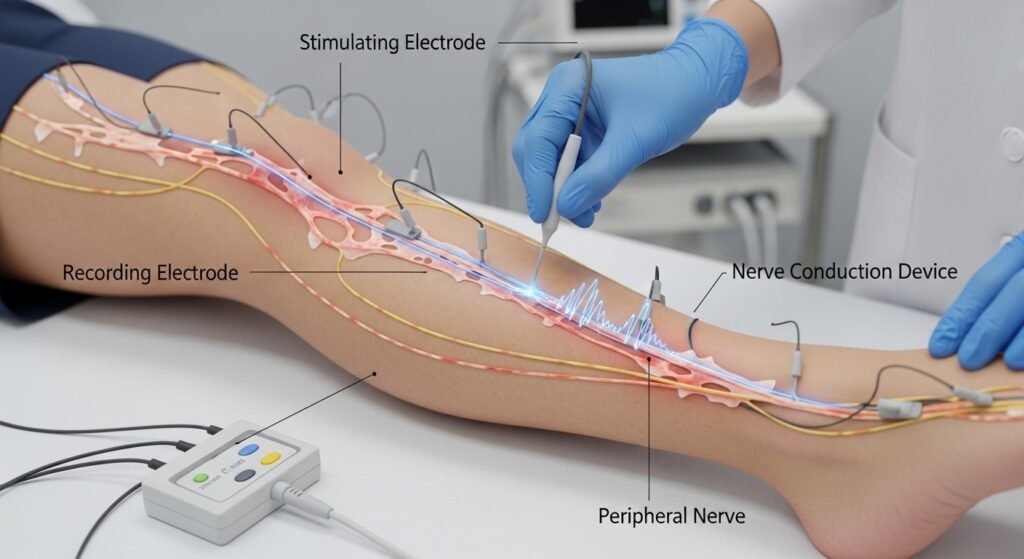
During NCS, small electrical stimuli are applied to skin overlying specific nerves, producing nerve impulses that are recorded at a distance. By measuring the speed of nerve conduction (conduction velocity) and the amplitude of the electrical response, the study identifies whether the nerve fiber (axon), its insulating myelin sheath, or both are affected — determining the type and severity of neuropathy. Multiple nerves in both arms and legs are typically tested in a comprehensive evaluation.
Electromyography (EMG)
EMG uses a thin needle electrode inserted into muscles to record electrical activity at rest and during contraction. Abnormal spontaneous activity (fibrillation potentials, sharp waves) indicates muscle denervation. The pattern of EMG abnormalities helps localize the site of nerve damage (anterior horn cell, root, plexus, or peripheral nerve) and distinguishes neuropathy from myopathy (muscle disease).
Common Conditions Diagnosed
- Carpal tunnel syndrome (median nerve compression at the wrist)
- Ulnar neuropathy (cubital tunnel syndrome)
- Peroneal nerve palsy
- Diabetic peripheral neuropathy
- Guillain-Barré syndrome
- Charcot-Marie-Tooth disease
- Radiculopathy (nerve root compression from disc herniation)
Conclusion
Nerve conduction studies and EMG provide objective, quantitative evidence of peripheral nerve and muscle dysfunction that clinical examination alone cannot fully characterize. If you have unexplained numbness, tingling, weakness, or muscle atrophy in your extremities, neurological evaluation including NCS/EMG provides the diagnostic precision needed to identify the cause and guide appropriate treatment.
FAQs – Nerve Conduction Studies
Q1. Do nerve conduction studies hurt?
A: The electrical stimuli used in NCS produce a brief, unpleasant but not severe “zap” or “jolt” sensation. The needle insertion for EMG causes brief sharp discomfort similar to a vaccine injection. The procedure is well-tolerated by most patients. Complete the study even if mildly uncomfortable — the diagnostic information is valuable.
Q2. How long does a nerve conduction study take?
A: A comprehensive NCS/EMG typically takes 60–90 minutes depending on how many nerves and muscles are tested. Your neurologist determines the extent of testing based on your symptoms and clinical findings.
Q3. Can nerve damage be reversed?
A: Peripheral nerves have some regenerative capacity — damaged axons can regrow, though recovery is slow (approximately 1mm per day) and may be incomplete. Myelin damage heals faster. The underlying cause of neuropathy must be treated to halt progression and enable maximum recovery.
Q4. Does diabetes cause nerve damage?
A: Yes. Diabetic peripheral neuropathy — caused by chronic elevated blood glucose — is the most common cause of peripheral neuropathy in developed countries, affecting approximately 50% of diabetic patients. Optimal blood sugar control is the primary strategy to prevent and slow progression.
Q5. What treatments exist for peripheral neuropathy?
A: Treatment is directed at the cause (glucose control for diabetes, vitamin B12 replacement for deficiency, immunotherapy for autoimmune neuropathies) and symptom management (anticonvulsants like gabapentin and pregabalin, SNRIs like duloxetine, topical agents for localized pain). Carpal tunnel and other compression neuropathies may benefit from surgical decompression.


