Food allergies affect approximately 32 million Americans and range from mild (itching, hives) to severe (anaphylaxis — a potentially fatal systemic allergic reaction). Unlike food intolerances (which involve digestive difficulty without immune involvement), true food allergies involve IgE-mediated immune responses that can be life-threatening. Allergy clinics and primary care providers use a combination of history, skin testing, blood testing, and oral food challenges to diagnose food allergies accurately. This guide explains how food allergy diagnosis works.
Clinical History: The Most Important Tool
A detailed allergy history — which specific food triggered the reaction, the type of reaction (hives, GI symptoms, breathing difficulty, anaphylaxis), how quickly after eating the reaction occurred (IgE-mediated reactions typically occur within minutes to 2 hours), reproducibility (does the same food reliably trigger the same reaction), and the amount of food required — provides the clinical framework that guides diagnostic testing. Not all self-reported food allergies represent true IgE-mediated allergies.
Diagnostic Tests
Skin Prick Testing
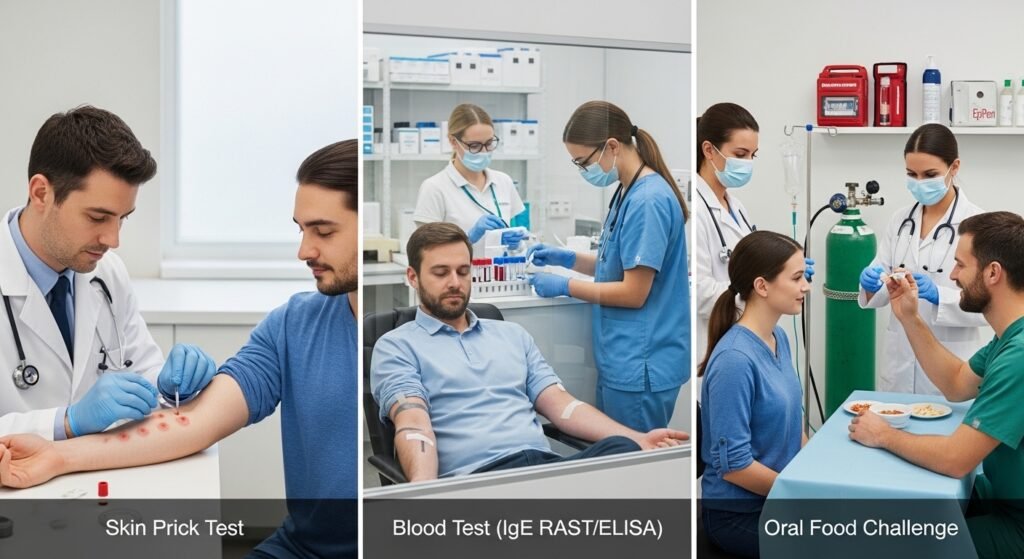
Small amounts of food allergen extracts are introduced to the skin via tiny pricks on the forearm or back. A raised wheal (bump) at a test site within 15 minutes indicates IgE sensitization to that food. Sensitivity varies by food — skin prick testing is most reliable for some foods (peanut, tree nuts, shellfish) and less reliable for others (fresh fruits, vegetables).
Specific IgE Blood Testing
Blood tests measuring food-specific IgE antibodies (ImmunoCAP or similar platforms) quantify sensitization to specific foods. Results above certain threshold levels are associated with higher probability of true allergy, though sensitization without clinical reactivity is common — positive tests must always be interpreted in clinical context.
Oral Food Challenge
The gold standard for food allergy diagnosis — supervised feeding of gradually increasing amounts of the suspected food under medical supervision with emergency treatment immediately available. An oral food challenge definitively confirms or refutes a suspected food allergy, and is particularly valuable for assessing whether previously diagnosed allergies have resolved (common in children with milk and egg allergies).
Conclusion
Accurate food allergy diagnosis matters — both for identifying genuine allergies requiring strict avoidance and epinephrine prescription, and for avoiding unnecessary dietary restriction based on positive tests without confirmed clinical reactivity. If you suspect a food allergy, a formal allergy evaluation through your clinic provides the accurate diagnosis needed to guide both safety and quality of life.
FAQs – Food Allergy Diagnosis
Q1. Is a positive food allergy test always meaningful?
A: No. Sensitization (positive test) without clinical reactivity is common — many people have positive IgE tests to foods they can eat without reaction. Test results must always be interpreted in the context of clinical history. An oral food challenge may be needed to confirm true allergy.
Q2. What are the Big Nine food allergens?
A: The most common food allergens in the US are peanut, tree nuts, milk, egg, wheat, soy, fish, shellfish, and sesame (added in 2023). These nine allergens account for approximately 90% of clinically significant food allergies.
Q3. Can food allergies develop in adulthood?
A: Yes. Adult-onset food allergies — most notably shellfish and tree nut allergies — are well-documented. New food allergies in adults warrant formal allergy evaluation.
Q4. What is the treatment for anaphylaxis from food allergy?
A: Intramuscular epinephrine (auto-injector, e.g., EpiPen) is the first-line treatment for anaphylaxis, followed by emergency services (911). All patients with confirmed food allergy at anaphylaxis risk should carry two epinephrine auto-injectors and have a written anaphylaxis action plan.
Q5. Can food allergies be cured?
A: Oral immunotherapy (OIT) for peanut allergy (FDA-approved product: Palforzia) desensitizes patients to peanut through gradual exposure. Many pediatric patients “outgrow” milk and egg allergies. Tree nut, shellfish, and fish allergies are typically lifelong. Research into immunotherapy for other food allergens is advancing.


