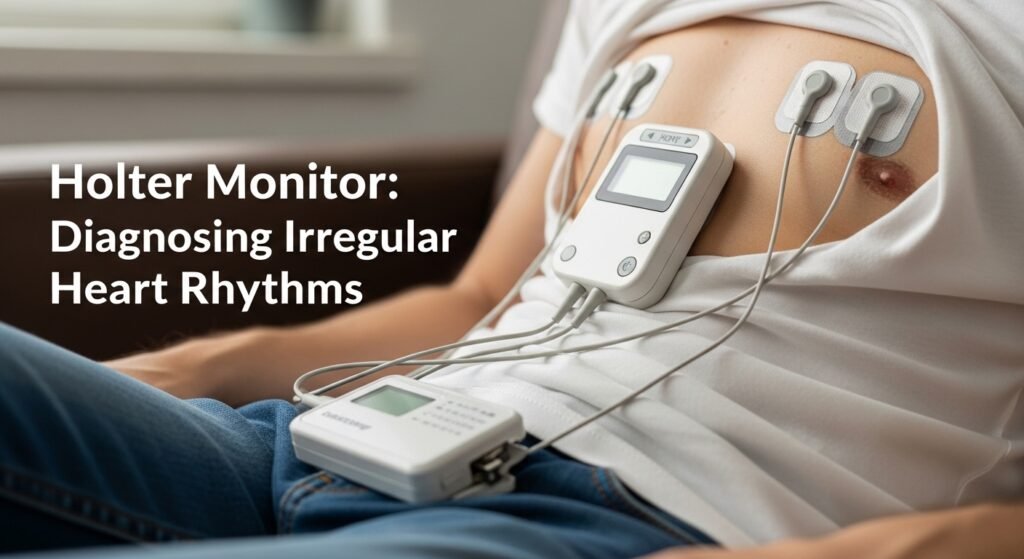
A Holter monitor is a small, portable device that continuously records the heart’s electrical activity for 24–48 hours (or longer with extended monitoring devices) while you go about your normal activities. Because many cardiac arrhythmias are intermittent — not present during the brief window of a resting ECG — ambulatory monitoring captures the rhythm abnormalities that cause palpitations, dizziness, or unexplained fainting. Medical and cardiology clinics order Holter monitoring when a patient’s symptoms suggest a cardiac rhythm disorder that the resting ECG did not capture. This guide explains Holter monitoring and related ambulatory cardiac monitoring.
What a Holter Monitor Records
The Holter monitor attaches electrode patches to specific chest locations connected by wires to a recording device worn on a belt or shoulder strap. It continuously records all cardiac electrical activity throughout the monitoring period. The recording captures heart rate throughout the day and night, any arrhythmia events, and the patient’s documented symptom diary — enabling correlation between symptoms and heart rhythm.
Conditions Diagnosed
- Atrial fibrillation and flutter — particularly paroxysmal episodes
- Supraventricular tachycardia (SVT)
- Ventricular tachycardia
- Significant bradycardia or heart blocks
- Correlation of palpitations with or without arrhythmia
- Assessment of pacemaker or ICD function
- Evaluation of unexplained syncope (fainting)
Extended and Event Monitoring
For symptoms occurring less than daily, a 24–48 hour Holter may not capture the event. Cardiac event monitors record only when activated by the patient during symptoms (event monitor) or automatically when abnormal rhythms are detected (loop recorder). Implantable loop recorders (ILR) — small devices implanted subcutaneously — provide monitoring for up to three years for very infrequent events.
Conclusion
Ambulatory cardiac monitoring bridges the critical gap between clinic-based resting ECG and the real-world heart rhythms patients experience during their daily lives. If you are experiencing palpitations, dizziness, or unexplained fainting episodes, a Holter monitor or related ambulatory monitoring study is an important diagnostic step your clinic can coordinate.
FAQs – Holter Monitor
Q1. Can I shower with a Holter monitor?
A: Most traditional Holter monitors should not get wet. Modern waterproof patch monitors allow showering. Ask your clinic specifically about water restrictions for your particular device.
Q2. What activities should I avoid during Holter monitoring?
A: Avoid MRI and other magnetic/electrical devices that could interfere with recording. Activities producing excessive sweating that loosens electrodes should be minimized. Continue all normal activities otherwise — the goal is to capture typical rhythms during typical daily life.
Q3. When will I get results from a Holter monitor?
A: After the monitor is returned, a cardiac technologist analyzes the recording (which may contain 100,000+ heartbeats), identifying arrhythmias and correlating them with the symptom diary. A cardiologist interprets the final report, typically available within 1–2 weeks.
Q4. What if nothing abnormal is found?
A: A normal Holter recording is valuable — it excludes significant arrhythmias during the monitoring period and, if symptoms occurred during monitoring without corresponding arrhythmia, provides reassurance that symptoms have non-cardiac causes. Extended monitoring or additional evaluation may be indicated if clinical concern persists.
Q5. Can a Holter monitor detect a heart attack?
A: Holter monitors are designed for rhythm analysis, not myocardial infarction detection. While some ischemic changes are visible on Holter recordings, it is not the appropriate test for evaluating suspected myocardial infarction — that requires urgent ECG and troponin testing.


